Book Appointment Now
Testicular Cancer
Testicular cancer is one of the less common cancers and most often affects younger men, typically between the ages of 15 and 49. It usually presents as a painless
swelling or lump in one testicle, or a noticeable change in the shape, size, or texture of the testicles.
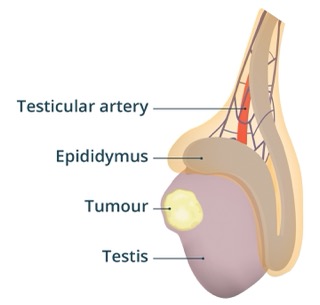
Being aware of what feels normal for you is important. Regular self-examination helps in noticing any changes early. If you observe anything unusual, consult a doctor promptly.
About the Testicles
The testicles are two oval-shaped male reproductive organs located in the scrotum. They have two major functions:
- Producing sperm, essential for male fertility
- Producing testosterone, the primary male hormone responsible for sexual development and male characteristics
Types of Testicular Cancer
Testicular cancers are categorized based on the type of cell in which the cancer originates.
- Germ Cell Tumors (95% of cases)
These are the most common and arise from germ cells—the cells responsible for producing sperm. Germ cell tumors are divided into two main types:
- Seminomas
- Increasing in incidence over the past 20 years
- Account for 40–45% of all testicular cancers
- Tend to grow more slowly
- Non-seminomas
- Include teratomas, embryonal carcinomas, choriocarcinomas, and yolk sac tumors
- Often grow and spread more quickly
Both seminomas and non-seminomas respond well to chemotherapy and have excellent treatment outcomes.
- Less Common Tumors
- Leydig Cell Tumors: 1–3% of cases
- Sertoli Cell Tumors: Less than 1% of cases
Most clinical discussions focus on germ cell tumors due to their high prevalence.
How Common Is Testicular Cancer?
- Testicular cancer is rare, accounting for only about 1% of all male cancers.
- Despite being uncommon overall, it is the most common cancer in men aged 15–49.
- It tends to affect younger men, unlike most other cancers.
- For reasons not fully understood, white men are at a higher risk compared to men of other ethnic groups.
Causes and Risk Factors
The exact cause of testicular cancer is unknown, but several factors may increase risk:
- Undescended testicle (cryptorchidism)
- Family history of testicular cancer
- Previous testicular cancer
- Abnormal testicle development
- Certain genetic conditions
- Ethnicity (higher risk in white race)
Treatment Options for Testicular Cancer
Testicular cancer is one of the most treatable and curable cancers, especially when detected early. Treatment depends on the type of tumor (seminoma or non- seminoma), the stage of the disease, and individual patient factors. Most patients have an excellent long-term outlook.
- Surgery (Orchidectomy)
The primary treatment for nearly all testicular cancers is surgical removal of the affected testicle.
This procedure is called a radical inguinal orchidectomy and is performed through a small incision in the groin.
Surgery allows:
- Confirmation of diagnosis
- Removal of the primary tumor
- Staging of the cancer
For early-stage cancers, surgery alone is often curative.
- Surveillance
For selected men with early-stage cancer, especially seminomas, active surveillance may be recommended after surgery.
This includes regular:
- Physical exams
- Blood tests (tumor markers)
- Ultrasound or CT scans
Many early-stage patients avoid further treatment with this approach.
- Chemotherapy
Chemotherapy is used for:
- Advanced-stage tumors
- Cancers that have spread to lymph nodes or other organs
- Non-seminomas with higher risk features
- Seminomas that require additional treatment
Common chemotherapy regimens include BEP (Bleomycin, Etoposide, Cisplatin) or variations depending on the case.
- Radiation Therapy
Radiation therapy is used mainly for seminomas, which are highly sensitive to radiation.
It may be used for:
- Early-stage seminomas
- Cancer spread to nearby lymph nodes Radiation is rarely used for non-seminoma tumors.
- Retroperitoneal Lymph Node Dissection (RPLND)
This is a specialized surgical procedure to remove lymph nodes at the back of the abdomen when:
- Cancer has spread to lymph nodes
- Residual masses remain after chemotherapy
- Non-seminomas have high-risk features
Performed by trained uro-oncology surgeons like Dr. Philip, RPLND can be an important part of curative treatment.
- Fertility Considerations
Because treatments like surgery, radiation, and chemotherapy may affect fertility, many patients choose to bank sperm before starting treatment.
This can be discussed early during planning.
- Overall Prognosis
Testicular cancer has one of the highest cure rates of all cancers.With prompt treatment, especially at early stages, success rates exceed 95%, and even many advanced cases are curable with modern therapy.

